Analysis by WorldTribune Staff, July 16, 2020
A Food and Drug Administration (FDA) safety review published on July 1 reported a total of only five adverse side effects among tens of millions of doses of hydroxychloroquine that were distributed to hospitals through the agency’s emergency use authorization.
“This suggests that the drug isn’t harmful to the vast majority of patients who are treated according to FDA guidelines,” Allysia Finley noted in a July 15 analysis for the Wall Street Journal.
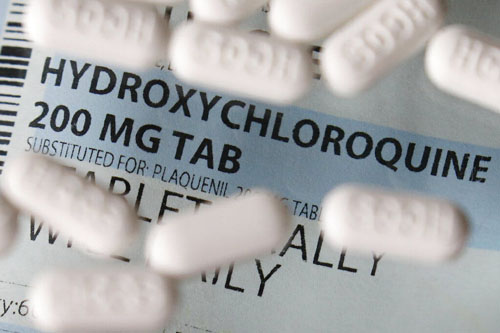 While the Left and major media played politics, thousands of coronavirus patients who could have been saved died, some analysts and health care professionals say.
While the Left and major media played politics, thousands of coronavirus patients who could have been saved died, some analysts and health care professionals say.
President Donald Trump has touted the effectiveness of the drug in treating coronavirus patients. So, naturally, Democrats, the vast networks enabling Joe Biden’s presidential candidacy, and their media allies denounced it.
Meanwhile, political pressure from the Left and the so-called “experts” they rely on to spread covid panic and attempt to keep the nation in lockdown led to the FDA suspending a permit for the use of hydroxychloroquine (HCQ) to treat covid patients.
The analysis by Finley, a member of the Journal’s editorial board, concluded: “Let doctors decide.”
Biden’s handlers sent the Democrat candidate out with a prepared statement saying that Trump “pushes dangerous, disproven drugs,” adding “our country is now stuck with a massive stockpile of hydroxychloroquine, a drug Trump repeatedly hailed.”
“Since every Trump action prompts a reaction, his political and media opponents launched a campaign to discredit the drug. This politicized environment has produced dubious science and erratic policy,” Finley noted.
When a WorldTribune contributing editor approached a primary care physician in the Raleigh, NC area for a prescription to hydroxychloroquine last week, he was told, “I would not be comfortable going that route. I have been getting letters from the state medical board.” The governor of North Caroline, Roy Cooper, is a Democrat.
Related: War on hydroxychloroquine: Texas doctor describes ‘alarming’ barriers to treating patients, May 15, 2020
On March 28, the Food and Drug Administration issued an emergency use authorization which gave hospitals the green light to treat coronavirus patients outside clinical trials using hydroxychloroquine donated by manufacturers to the national stockpile. But on June 15 the agency rescinded the authorization. “In light of ongoing serious cardiac adverse events and other potential serious side effects,” the FDA announced, “the known and potential benefits of . . . hydroxychloroquine no longer outweigh the known and potential risks for the authorized use.”
But, Finley noted, “the scientific basis for the revocation now appears faulty. Most studies didn’t adjust results for confounding variables such as disease severity, drug dosage or when patients started treatment. Two new peer-reviewed studies find that HCQ can significantly reduce mortality in hospitalized patients. With hospital beds filling up across the American South and West and a limited supply of Gilead Sciences’ antiviral remdesivir, the FDA should reinstate its emergency-use authorization for HCQ.”
HCQ has been safely used for decades to treat patients with lupus and rheumatoid arthritis, both inflammatory autoimmune conditions. The drug has also been found to interfere with the novel coronavirus’s replication in vitro, and studies this spring from France, Brazil and China showed the drug might help moderately ill patients.
In late May, the medical journal Lancet published a large-scale international study that claimed hospitalized coronavirus patients treated with hydroxychloriquine were 30 percent more likely to die. The Lancet retracted the study on June 4 after more than 120 scientists pointed out significant flaws in the data and methodology. The source of the raw data refused to share it with independent reviewers.
“Nonetheless, the anti-Trump media claimed vindication later that day when the New England Journal of Medicine published a randomized trial that concluded HCQ didn’t prevent illness in people who had been exposed to the virus,” Finley wrote. “The study’s raw data showed that people who took HCQ within two days of exposure were 38% less likely to develop symptoms. But a third of subjects in the trial took the drug four days after exposure, which obscured its benefits. Since the average viral incubation period is five days, starting the drug four days after exposure is unlikely to do much good.”
On June 5, University of Oxford researchers reported that a midpoint review of their HCQ trial had found no clinical benefit. “This result should change medical practice worldwide,” Oxford epidemiologist Martin Landray declared in a press release.
However, Finley noted, the Oxford team “didn’t release its raw data, so it’s impossible to know whether the drug may have helped a subset of patients, such as those treated at an earlier stage of the disease or with elevated biomarkers of inflammation. The trial’s protocol also called for dosages two to three times as high as those recommended by the FDA’s emergency use authorization.”
The FDA revoked its authorization to treat covid patients with hydroxychloroquine 10 days later.
The FDA cited the New England Journal and Oxford work as well as a British Medical Journal study from China that purportedly found no benefit from the drug. Yet an April draft of the last study concluded that HCQ accelerated “the alleviation of clinical symptoms, possibly through anti-inflammatory properties” and “might prevent disease progression, particularly in patients at higher risk.”
On June 30, the first of the new studies showing benefits from hydroxychloroquine appeared in the Journal of General Internal Medicine. The study found patients treated with the drug at New York’s Mount Sinai Health System hospitals were 47 percent less likely to die after adjusting for confounding variables such as underlying health conditions and disease severity.
“Notably, Mount Sinai’s treatment protocol called for lower dosages than in the Oxford trial, and patients on average were treated within one day of hospitalization,” Finley noted.
The second study showing HCQ’s benefits, published July 1 in the International Journal of Infectious Diseases, found that patients treated with the drug at Henry Ford Health System hospitals in Detroit were 50 percent to 66 percent less likely to die after adjusting for confounding variables including other treatments.
Finley pointed out that “Nearly all patients began treatment within two days of admission, received dosages that hewed closely to FDA guidelines, and were continuously monitored for cardiac arrhythmias.”
The Henry Ford doctors noted: “Our patient population received aggressive early medical intervention, and were less prone to development of myocarditis, and cardiac inflammation commonly seen in later stages of COVID-19 disease.”
“With hundreds of Covid-infected Americans still dying each day, the FDA should let physicians decide whether to treat patients with HCQ based on their experience and scientific evidence. Leave politics out of it,” Finley concluded.
Intelligence Brief __________ Replace The Media
